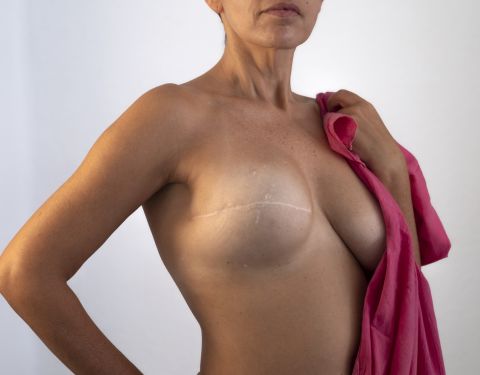
Satisfaction is one of the essential dimensions of quality measurement. That’s why after several experimental years and in addition to its already existing evaluation mechanisms – HAS has launched a national measure of inpatient satisfaction.
Measure satisfaction to improve the quality of care and information.
Patient satisfaction in France. How does it work?
Since September 2015, every patient is asked to communicate his email address upon admission in an institution of medicine, surgery, and obstetrics. Then, for any hospitalization of more than 48 hours, the patient receives by email two weeks after his release, a link to a secure and anonymized satisfaction questionnaire.
The 15-day period makes it possible to carry out the “cold” survey, with hindsight and at home, using a comprehensive questionnaire to provide accurate information to health institutions to identify improvement.
In about 10 minutes, the patient (or his entourage) can give his opinion on four dimensions of his hospitalization:
- His reception in the establishment;
- His care;
- His room and his meals;
- The organization of his release.
How are these results for patient satisfaction used?
The anonymized results of these questionnaires are passed on to health facilities so that they have feedback from their patients, understand their strengths and weaknesses and know how to improve. They have quantitative data for this purpose as well as verbatim of the patients.

Patient record information
The patient’s file is the place of collection and preservation of administrative, medical and paramedical information, formalized and up-to-date, registered for any patient who has visited, for whatever reason, health institution.
It is a fundamental tool for monitoring patients on a daily basis, coordination between different health professionals and continuity of care after hospitalization. It is a reflection of clinical practices and their quality. The 2016 results show that for all types of activity, almost all patients’ files are organized.
Assessment and management of pain
The management of pain is a public health priority and an obligation enshrined in the French Health Code. “Everyone has the right to receive care to relieve pain.” Pain slows down and complicates the recovery of the patient. This is why health professionals must systematically evaluate it and the patient must be relieved when he suffers.
Assessments and medical examination of the patient
Upon admission to a health facility, the patient must be examined to review his / her situation, medical history, etc. but he must also be the recipient of the necessary information on his care. Despite progress, this review is not yet systematic in all health facilities.
Specific assessments for good management
Depending on the case, special assessments must be carried out for each patient in order to:
– check his or her health status during treatment in the facility (for example, progressive surveillance symptoms, monitoring of weight or temperature, all of which may constitute warning signals);
– check that the proposed treatment is appropriate (for example, to evaluate the modalities of drug treatments of the patient);
– prevent certain consequences of hospitalization (for example, assess the risk of pressure sore for patients who will be bedridden for long periods of the day and put in place preventive measures).
If the results show the progress of the practices in some establishments, others still have a margin improvement, in particular, assessment of the risk of eschar in short-stay; weight control in hospitalization at home or psychological assessment in follow-up care and rehabilitation, according to the clinical situation of the patient.

Respect for patients’ rights
Each health facility must organize itself to respect the rights of the patient: the right to information on his condition and care offered to him, the right to appoint a person of trust, participation in his responsibility, privacy, confidentiality, etc.
Feedback from patients shows that more than 70% of patients received spontaneous explanations on their state of health, treatment, and care. Half of the patients wished to participate in decision-making about their care, 7 out of 10 were able to do so on a regular basis.
HAS also analyzed other dimensions such as the agreement and the association of the patient and his entourage in the special cases of home-based hospitalization (which mobilizes the patient’s relatives throughout the hospital stay), follow-up and rehabilitative care.
Mention of the person of trust or designated persons in mental health
Since 2005, the Public Health Code has allowed each patient to appoint a person of trust who can be consulted by the doctors if the patient is no longer in a position to give his opinion. It’s up to the professionals in the institutions to ask patients if they have appointed a trusted person and if so, explain to them the interest of this approach.
Hospital discharge and continuity of care
Hospital discharge is a time when the risks of continuity of care are important with consequences of unplanned rehospitalization, worsening of the patient’s state of health, unnecessary anxiety but also patient dissatisfaction.
Drugs
Medication management in a health facility must ensure that the patient has the right medication at the right dosage, in the right way, in the right conditions. In the hospital, the drug follows a long circuit before reaching the patient (prescription, preparation, storage, dispensing, and administration to the patient).
If the drug prescriptions are globally recorded and in a correct manner, the results measured in 2016 remain clearly insufficient concerning the quality of the medications, exit treatments, and their communication.
What is HAS doing to help health facilities to improve their outcomes?
– Organization of the outing and care path
HAS has carried out various work to determine the content of the exit document with which the patient must leave the hospital. It has developed a repository on the hospital discharge document superior to 24 hours. It has also put in place an indicator that looks at the quality of the document given to patients.
The document is given on the day of the hospital discharge and its content respects the five compulsory categories (reason for hospitalization, a medical summary of the stay, results of complementary acts and examinations, prescribed medical treatments, recommended a medical follow-up.
It has also developed various tools adapted to the different transitions of sick people. It set up an outpatient checklist and developed a model of the personalized program of care adapted to the elderly.
It has also developed specific end-of-life documents to improve the release from the hospital and facilitate home care for adult patients. Finally, to improve the coordination of care, the tracer patient method has been extended to the city.
– Securing medical care in a health facility
HAS has published numerous guides and tools on this theme, which remains a subject of dysfunctions too common in institutions:
- tools to self-evaluate and secure the stage of drug administration in institutions;
- a guide to limit work interruptions and limit their impact, i.e. when the person preparing the drugs is interrupted in his task to respond to a colleague, go to the bedside of a sick person, etc.
HAS also conducted work on the reconciliation of drug treatments, showed its interest in the prevention and interception of medication errors.
HAS has just completed a guide on the implementation of treatment reconciliation medications in health establishments taking into account the city-hospital including tools to enable the replication and deployment of the conciliation procedure in all health facilities that wish. This guide will be published very soon.
– Operating room
HAS has adapted and deployed the checklist to the operating block in all French health. Its 2016 version is adapted to infant surgery. This new version replaces the 2011 version of the documents. In order to promote its appropriation by professionals, this generic checklist can be adapted according to the context and specificities of the disciplines.
It also produced tools around cooperation between surgeons and anesthetists because the quality of teamwork including communication between anesthetists and resuscitators and surgeons represents a major stake for the safety of the patient.
– Patient identification
The checklist deployed by HAS includes elements of vigilance on the identity of patients and their verification.
In general, it can be noted that verification carried out by HAS was successful. Verification once again confirmed the highest level of French medicine. It is especially pleasant to note the constant progress of France in the field of medicine.
While others are satisfied with simply good results, the French are doing everything possible to become the best. And, in order to become the best, you need not only to find your shortcomings, correct them but also you need to constantly improve.
Everyone knows that the sky is the limit, therefore the desire to be the best implies constant work on yourself. Fortunately, in France, medicine is maintained at the state level, which gives hope to look to the future with optimism!